The Part D standard benefit design still has a deductible, initial coverage phase, coverage gap discount phase, and a Catastrophic phase. None of that has changed. However, there are two elements of the redesign that can negatively impact drug revenue:
Manufacturers now must provide a 20% discount when a patient enters Catastrophic Phase coverage
In the previous design, Medicare and Part D Plans paid 95% of drug costs in the Catastrophic phase while the patient paid the last 5%. Manufacturers covered none of those costs. This meant drug manufacturers were paid near the drug’s list price (minus rebates and other deductions, of course). The new 20% reduction is the first time manufacturers have been required to offer a discount in the Catastrophic phase.
This year, patients are required to cover about $7,050 in total out-of-pocket drug expenses. In 2025, patients will have their max-out-of-pocket (MOOP) lowered to $2,000.
Because of the lowered max-out-of-pocket threshold, patients will move through the phases of coverage much more quickly. Figure 1 (below) shows a 25% patient share in Initial coverage as well as in the Coverage Gap. With a $2,000 MOOP, patients will not be in the Coverage Gap very long. While this is truly a great benefit for patients, it means more prescriptions will be written in the Catastrophic phase and therefore require a 20% discount from the manufacturer and a 20% contribution from the Plan.
Figure 1: Part D Standard Benefit- 2022 vs. 2025
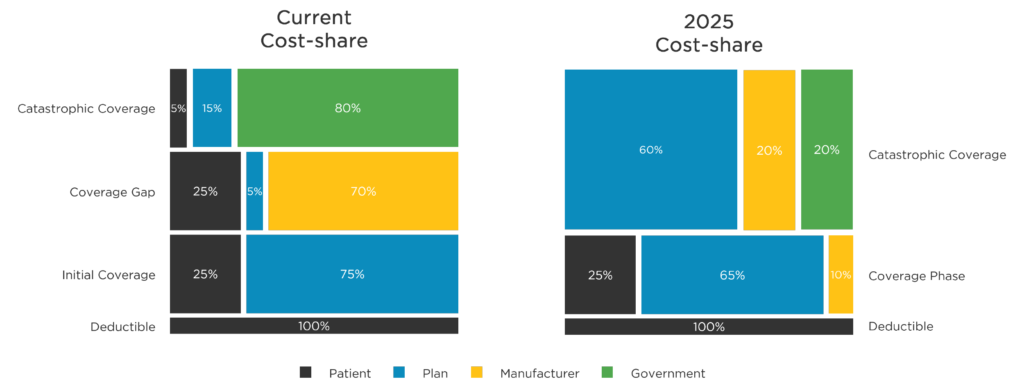 Figure 1: Note the new 20% obligation for manufacturers in the Catastrophic phase
Figure 1: Note the new 20% obligation for manufacturers in the Catastrophic phase
Impact on Pharma
Some of the impacts are obvious, while others are not:
As we noted, the discount is 20%. A less obvious impact is seen when drug rebates are factored in. It is not unusual for manufacturers to realize only 50% net revenue on a prescription, after rebates and other reductions. Using a short math equation as an example:
- Assume a $100 list price for a prescribed drug
- Let’s also assume a 40% rebate (not unusual). This leaves $60 in revenue
- When the patient enters the Catastrophic phase, the manufacturer must offer 20% off the list price, NOT the post-rebate value of $60
- So, after taking $20 off the list price and paying the rebate, a manufacturer is left with $40 net revenue
This scenario is similar to the “double-dipping” seen in Medicaid. One prescription to a Medicaid beneficiary can sometimes result in a rebate paid to the Managed Medicaid payer as well as a standard rebate of 23.1% paid to the state Medicaid program. The laws are designed to prevent this, but it still happens. It could easily happen under the new law as well.
Even low-cost drugs are affected
Pricey drugs can obviously drive a patient to the Catastrophic phase quickly. But even lower-cost drugs can be impacted by the $2,000 MOOP. Polypharmacy is common in Medicare patients, and the cost of several monthly prescriptions can add up quickly. This means even the $100/month prescription we used as an example can run into the 20% discount requirement.
Part D Plans may restrict access to more drugs
In the current Part D design, Plans must cover 70% of drug costs in the Initial Coverage phase, 5% in the Coverage Gap, and 15% of drug costs in the Catastrophic coverage phase. Plans have devised formularies and other strategies that are intended to facilitate a patient’s movement through Initial Coverage so they get to the Coverage Gap (and the 5% Plan share).
Now, however, Plans must cover 20% of drug costs in the Catastrophic phase. In addition, with a $2,000 MOOP, patients will spend very little time in the Coverage Gap where Plans only have to cover 5% of drug costs. This may incentivize the Part D Plans to tighten their cost containment strategies. More restrictive formularies, more step edits, and other measures may be seen in the marketplace, thereby restricting access to many drugs.
Conclusion
Changes in the Part D benefit design will have a significant impact on drug revenues. Another consideration is that more drugs will be impacted by these Part D changes than will be impacted by Medicare price negotiations. These impacts will absolutely be felt behind the scenes in places like the rebate negotiation rooms populated by payers and manufacturers.
Join our free webinar on Wednesday August 31, where we will have a discussion on predicting how pharma may react to these substantial changes